Lupus is a chronic autoimmune disease which can affect various systems in the body. Autoimmune diseases cause the body to attack its own cells as if they were foreign pathogens. This can result in a wide assortment of physical symptoms, largely depending on which system (e.g., central nervous system, renal system, cardiovascular system) is most “under attack.” Antibodies are produced by the body which attack healthy cells and tissues, and these hyperactive immune responses can be extremely damaging to many parts of the body. When essential organs are attacked by the disease, lupus can be life threatening. Known not-so-affectionately as “
The Great Imitator,” the disease has been historically difficult to diagnose and treat, due in part to its symptoms’ similarities to a host of other illnesses.
Patients’ experiences with lupus differ, but in general signs and symptoms frequently include:
- Fatigue
- Fever
- Weight loss or gain
- Joint pain, stiffness and swelling
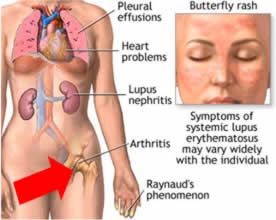
- Butterfly-shaped rash (malar rash) on the face that covers the cheeks and bridge of the nose
- Skin lesions that appear or worsen with sun exposure
- Mouth sores
- Hair loss (alopecia)
- Fingers and toes that turn white or blue when exposed to cold or during stressful periods (Raynaud's phenomenon)
- Shortness of breath
- Chest pain
- Dry eyes
- Easy bruising
- Anxiety
- Depression
- Memory loss
Mayo Clinic
Below are the four main types.
- Discoid lupus erythematosus or cutaneous lupus. This type affects only the skin. People with discoid lupus, experience a circular rash on the neck, face and scalp. Some of people with discoid lupus may develop systemic lupus erythematosus, though it is not possible to calculate who will develop severe form of lupus.
- Systemic lupus erythematosus. The body systems most commonly involved includes the kidneys, skin, blood, joints, and lungs. It can affect nearly any part of your body. When people talk about lupus, they’re usually referring to systemic lupus erythematosus.
- Neonatal lupus. A mother with certain antibodies that are linked to autoimmune diseases can pass them to the developing fetus, even if the mother has no signs or symptoms of an autoimmune disease. This is a rare form of lupus that affects newborn babies. The antibodies can cause neonatal lupus. A baby with neonatal lupus may experience a rash in the weeks following birth for last several months before the disease is disappearing.
- Drug-induced lupus erythematosus. It can occur after some people take certain prescription medication. Antibiotic drugs such as, amoxicillin, ampicillin, and cloxacillin or sulfa drugs such as trimethoprim-sulfamethoxazole, sulfisoxazole, and sulfasalazine may cause lupus. Not everyone who takes these medications develops lupus. Signs and symptoms usually go away when the taking of the medication is stopped.
Autoimmune Disease Blog
IMMUNE NETS
White blood cells called neutrophils from lupus patients (left) and healthy people (right) are shown after attack by lupus antibodies. Healthy neutrophils expire in an orderly manner, but lupus neutrophils spill their contents into web-like structures (shown) that trigger production of inflammatory proteins.
Science News
Scientists still aren’t sure what causes lupus, but fascinating new research has been conducted which shows how immune cells called neutrophils may be involved.
Short-lived but populous immune cells called neutrophils and the cellular flotsam they sometimes release might play an important role in lupus. Neutrophils from lupus patients give rise to microscopic nets, made of unwound DNA and proteins, that may trigger the inflammation characteristic of this autoimmune disease, according to two laboratory studies released online March 9 in Science Translational Medicine.
[. . .]
Neutrophils, the most abundant white blood cells, have long attracted researchers’ interest. Patients often have a shortage of normal neutrophils in the blood and an excess of immature neutrophils, which get rushed into duty when the supply of mature cells runs low, says Virginia Pascual, a pediatric rheumatologist at the Baylor Institute for Immunology Research in Dallas. But neutrophils’ role in lupus has never been clarified.
[. . .]
Neutrophils normally serve on the front lines against disease. But in one of the two new studies, Pascual and her colleagues show in lab tests that exposing neutrophils from lupus patients to abnormal antibodies, also from lupus patients, induces the neutrophils to die rapidly in culture. What’s pivotal is how the cells expire: The neutrophils’ components are extruded from the cell and form neutrophil extracellular traps, or NETs, weblike structures that comprise unwound strings of DNA, proteins and other cell components.
When neutrophils from healthy people were exposed to the rogue lupus antibodies, the cells didn’t release their contents in NETs.
Science News
I’m pushing fair use, so please read the article for the second study.
Though the exact causes of lupus remain a mystery, several patterns are clear. At this time, it is believed that one cannot inherit lupus directly, but that a genetic predisposition to it, added to environmental factors, can result in the expression of the disease. There are a number of risk factors, including being female, Latino, African American, Asian American, or extensively exposed to sunlight. African Americans and Latinos appear to be most heavily affected by lupus, as they are both more likely to develop it, and more likely to experience complications associated with the disease.
The study, published in the summer issue of the journal Ethnicity & Disease, was based on six years of data from lupus patients in Dallas-Fort Worth-area hospitals. The researchers found that white patients were half as likely as other ethnic groups to have the disease.
Hispanic women tended to have the most severe lupus cases, which often were complicated by the presence of other diseases. These women, for example, had a 61 percent greater chance of having kidney inflammation -- or nephritis -- in addition to lupus, and a 55 percent greater likelihood of also having diabetes, the study found.
In all, Hispanic and black patients with SLE were twice as likely as whites to also have nephritis, kidney failure and inflammation of the heart lining, all of which complicate the treatment and severity of the disease, according to the researchers.
Latino Med Journal
Coping with this disease can be an incredibly complex, difficult endeavor, though a number of treatment methods are available. One problem in treatment is that many drugs we have for use in these cases suppress the immune system, opening the door to possible infections. Striking a balance between sufficient immune system suppression to ease the symptoms of lupus without leaving patients vulnerable has proven an arduous task. But in an exciting new development, for the first time in 50 years the FDA has approved a new drug to treat lupus. Called Benlysta, the drug seeks to decrease the over-activity of the immune system without excessively compromising the immune system as a whole.
Doctors said that for many mild to moderate cases of lupus the experimental, injectable drug called Benlysta was able to suppress the immune system, just enough.
"It basically takes the sort of hyperactive part of the immune system and decreases that hyperactivity," said Dr. Mary Anne Dooley with the University of North Carolina, Chapel Hill.
Some said the drug's benefits are mild and others said Benlysta has worked to keep flare-ups under control.
MSNBC
Despite the hope offered to some patients, the treatment
is not effective for some of the people who need it most. In the most severe, life-threatening cases, it does not appear effective, and African Americans unfortunately do not seem to respond well to the drug. In light of the latter concern, the FDA has announced that researchers will need to conduct further studies focusing solely on African Americans.
Interesting developments here, but plenty of shortfalls. We can only hope that further research into the mechanisms of this drug will lead to new discoveries that will enable scientists and doctors to treat a broader range of people.


