Yes, I purposely parodied the name of the cult zombie/pandemic movie 28 Days Later to make a point. We are 28 MONTHS LATER in the battle against COVID. While we have made some progress, too many are declaring a victory too early. #CovidIsNotOver, and in fact another nasty wave could be coming in April/May, thanks to the Omicron BA.2 subvariant. Where do I get the evidence for this prediction? These four reasons explain it.
First, what is happening in Hong Kong shows that the unvaccinated and not boosted are at great risk. Those that shun pandemic precautions are also at greater risk. BA.2 is just as lethal to people not taking the pandemic seriously!
Next, cases in Europe are starting to spike once again. Perhaps it is just noise, but many nations having a spike at the same time is too much of a pattern not to say the BA.2 wave is coming.
Look at the trend of hospitalizations in England (see below) that Dr. Fiegl-Ding has highlighted in this twitter thread I unrolled.
 Number of admissions to the hospital in each age category is starting to spike again.
Number of admissions to the hospital in each age category is starting to spike again.
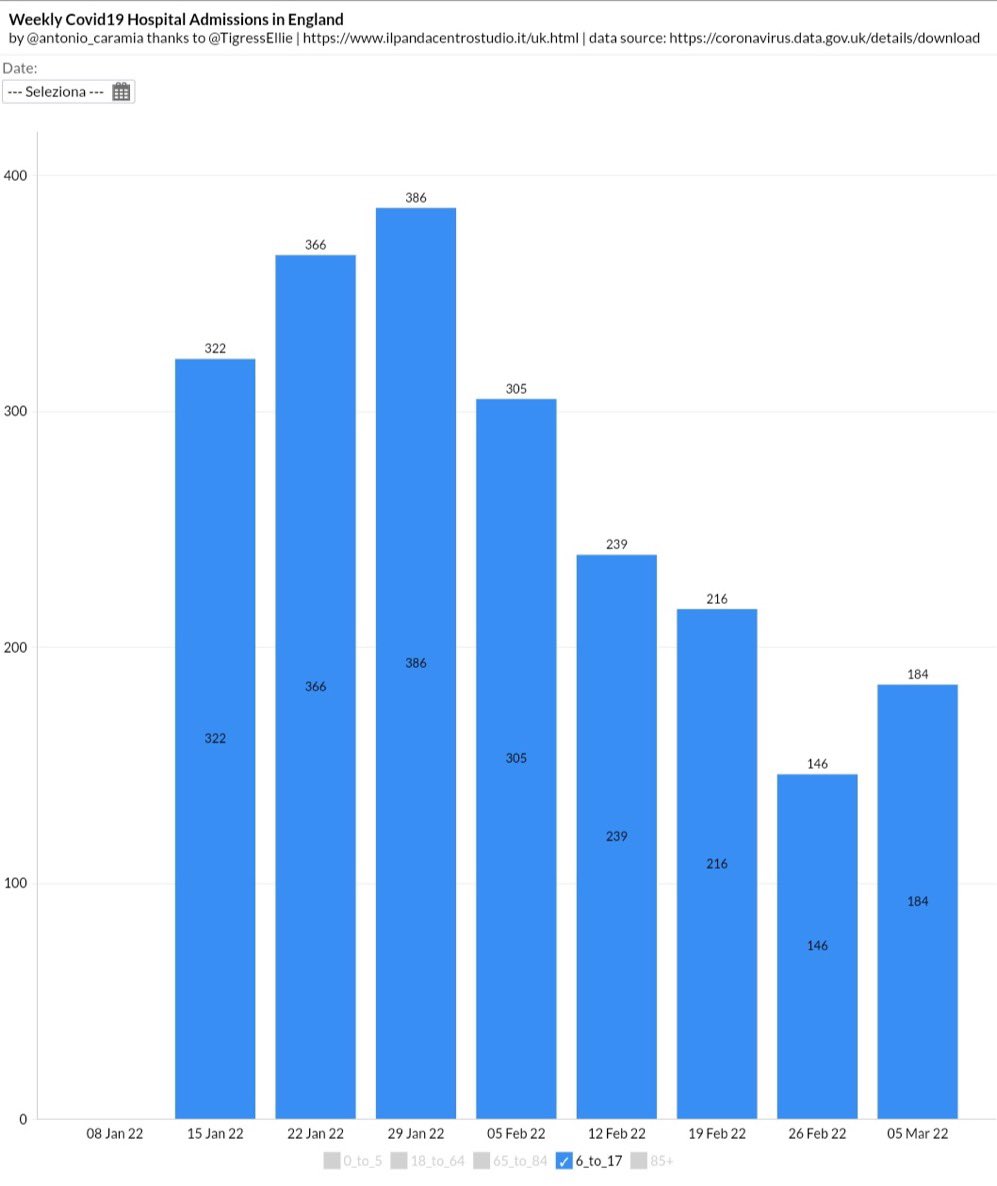 Hospital admissions going up once again. Deaths are sure to follow, as they are the lagging indicator.
Hospital admissions going up once again. Deaths are sure to follow, as they are the lagging indicator.
After that, the projected trend of US cases is showing a plateau right now, but lax precautions combined with waning immunity predict another surge of BA.2 starting in April or May. Remember, what happens in Europe has happened here 4-6 weeks later repeatedly. It isn’t farfetched to think it will follow the same pattern.
Finally, a study out of Qatar shows that BA.2 has 10x the viral load of BA.1 Omicron. This is why it outcompetes the other subvariant, and why when booster immunity wanes, we shall have another wave. Luckily, infections + boosters will make the cases milder still. But we are pressing our luck that it doesn’t mutate into something that evades the vaccines.
Future mutations in BA.2 may be what renders current vaccines only marginally effective, as this thread unroll shows. BA.2 may even be picking up mutations that made Delta so lethal!
Highlighted by me:
Omicron: BA2, Alarming new study shows BA2 may lead to '27x increase in vaccine-breakthrough capabilities': '30% more capable' to escape vaccines. 4.2x more contagious than Delta—20x more infectious than original strain & has 28 'distinct mutations'...
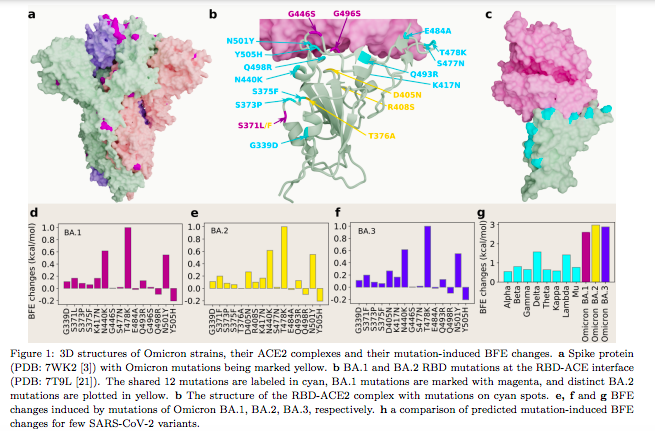 Lots of spike protein changes in BA.2, even when compared to original Omicron (BA.1)
Lots of spike protein changes in BA.2, even when compared to original Omicron (BA.1)
The researchers believes that these mutations, especially in RBD, allow for much greater infectivity and immune escape.
 The spike protein is like a key fitting into a lock. BA.2 may be the best lockpick yet.
The spike protein is like a key fitting into a lock. BA.2 may be the best lockpick yet.
However, the battle against COVID is so focused upon the death toll that it is missing the real enemy in this battle. Continue over the fold to see who the real villain of this medical drama is 28 MONTHS LATER.
“We Don’t Talk About Bruno COVID”
Musical break. Substitute “Covid” for “Bruno” and it still works perfectly as this parody shows! HT to Love the USA for sharing!
Many sufferers of Long COVID suffer in silence. Doctors disbelieve survivors and chalk it up as “imaginary” or “psychosomatic”. “You’re just a long hauler, they get better eventually”. Family and friends make assumptions that they are depressed (often true), lazy (not true AT ALL), or faking it (why would we want to be miserable all the time?).
Their disability makes it difficult on some days to get out of bed, let alone interact with other people. This puts many Long COVID sufferers in extreme isolation for extended periods of time. That’s on top of the politicization of the virus by the Tangerine Terror in the early days, which sprouted the amusing yet depressing Herman Cain Awards and the “Anti-Vax Chronicles” here. If you are born in the wrong area, your support system crumbles when “COVID is a Chinese bioweapon that doesn’t exist but hospitals kill people to profit off of it” or something along those lines...
People have to turn to Facebook, which is a fount of misinformation and quack cures. The (at first) respectable long hauler group I joined became a place to hawk ivermectin, hydroxychloroquine, and essential oils. People are afraid and desperate to try anything — ANYTHING — that may work. Long haulers want their old life back and don’t achieve it, and “We Don’t Talk About Long Covid” becomes a set in stone reality.
Here's just one personal account of what life with Long Covid is like.
Laurel Murphy contracted COVID-19 in December 2020, and her condition quickly worsened. Over the course of two weeks, Murphy progressed from a fever, intense vomiting and body aches to an acute shortness of breath that led to an emergency room visit and a monthlong stretch at home during which she required oxygen.
“I was severely dehydrated and was having trouble walking. We live in a tiny ranch house, and I couldn’t make it from the bedroom to the bathroom on my own,” Murphy said recently by phone. “My oxygen levels were so low that they dropped into the 60s. (A healthy blood oxygen level varies between 75 and 100 millimeters of mercury). It was the strangest thing, where this weird, dark feeling just came over me, and I don’t even know how to describe it, but it was like, ‘I’m not going to make it.’”
Gradually, though, the supplemental oxygen took effect, along with a regimen of steroids, fever reducers and cough suppressants that forced Murphy to take a different medication every couple of hours around the clock. Over the course of a month, she started to trend in the right direction...
SPOILER ALERT: it went downhill again from there.
So now, I *am* going to talk about “Bruno”.
Long Covid is very prevalent across the globe and does not always go away
The enemy within is Long Covid, or the COVID-19 symptoms that seem to linger long after you have tested negative for the initial infection of virus. Whether it is a cytokine storm that triggers multiple organ damage, or virus particles left over that the immune system attacks, we don’t know yet. It could be both, it could be neither. More scientists are researching Long Covid than any other chronic illness in history. Sadly, too many PCPs dismiss the symptoms as “in their heads” or “will go go away”. That simply isn’t the case!
It is suspected that about 30% of people infected with COVID develop long COVID. Sometimes, the symptoms go away after a few months, but in other people the symptoms do NOT go away. Senator Tim Kaine is an example of a two year long COVID sufferer. I am a 16 month long COVID sufferer. And we are not alone.
About 30% of workers in the UK suffer from a long term illness, a huge spike in 28 months. Long Covid is the suspect in the dramatic increase. This hidden toll may be behind the worker shortage as long haulers like me drop out of the workforce. Even “mild” cases will lead to more sick days, disability claims, higher insurance costs, and likely a lowering of life expectancy.
Kids are being set up for a lifetime of chronic illness and trauma. Could it be like polio or chickenpox/shingles and do irreparable harm in old age by hiding in the body? We don’t know yet.
long covid causes problems throughout the entire body
- Long Covid changes the immune system. Long Covid seems to happen because of continued immune system stimulation. My own blood work has a similar pattern where I have too many immature T cells and not enough of the specialized T cells. Also explains why I have developed an autoimmune disorder.
- Long Covid attacks the lungs and causes shortness of breath. Gas exchange is more difficult because those regions of the lung are infected and destroyed by the autoimmune response. It took a very special CT machine to find out the TRUE extent of the damage.
A new type of imaging technology has detected lung damage in patients suffering from the long-term effects of COVID-19. The weakened lung function was not visible on standard MRI or CT scans and its detection will help clinicians understand the persistent breathing impairments seen in patients with long COVID.
The phenomenon of long COVID is still a bit of a mystery, with researchers only just beginning to grasp the long-term implications of infection with this novel coronavirus. Fatigue and breathlessness are two of the most commonly reported lingering symptoms in COVID-19 patients following discharge from hospital. Yet standard MRI and CT scans often deliver normal results leaving many clinicians unable to empirically explain these patient symptoms.
- Your arteries and heart can be restricted by Long Covid, which means that increased blood flow cannot happen when it is needed. The endothelial cells surround your arteries and allow the immune system to properly function. COVID seems to infect and change them, leading to problems with autoimmune disease and restricted blood flow. Heart disease and heart attacks are a great risk of COVID even a year after the infection.
- Long Covid can mess with liver function. Your liver becomes fatty which can lead to metabolic changes, cirrhosis, and death.
A majority of long-COVID patients who had been hospitalized for severe COVID-19 illness had metabolic (dysfunction)-associated fatty liver disease (MAFLD), a retrospective study from Italy found.
In an analysis of 235 patients presenting to a post-acute COVID syndrome (PACS) clinic in Italy, 55.3% had MAFLD during follow-up as compared to 37.3% upon their initial hospital admission (P<0.001), reported Paolo Raggi, MD, of the University of Alberta in Edmonton, and colleagues.
"MAFLD was a highly prevalent condition in our cohort of survivors of hospitalized patients with COVID-19, and we speculate that it may be considered as an independent PACS-cluster phenotype, potentially affecting the metabolic and cardiovascular health of patients with PACS," the group wrote in Open Forum Infectious Diseases.
- Long Covid can lead to kidney damage or kidney disease. The kidneys help filter out toxins, and small blood clots block the passages to the kidney that do this function. This is a silent killer, as there usually is no pain or sign of a problem until it is too late.
Research continues to mount indicating that many people who’ve had COVID-19 go on to suffer a range of adverse conditions months after their initial infections. A deep dive into federal health data adds to those concerns, pointing to a significant decline in kidney function among those dubbed COVID-19 long-haulers — and even among those who had mild infections of the virus.
The data, plumbed by researchers at Washington University School of Medicine in St. Louis and the Veterans Affairs St. Louis Health Care System, show that those infected with SARS-CoV-2 are at an increased likelihood of developing kidney damage as well as chronic and end-stage kidney diseases.
- Long Covid can trigger diabetes, even if the person was completely healthy before. It is believed that the autoimmune response kills insulin producing cells and also increases insulin resistance in those with pre-diabetes.
For some people, surviving COVID-19 may lead to lasting medical concerns, including newly diagnosed diabetes. This is a chronic disease that happens when your blood glucose, also called blood sugar, is too high.
The pancreas makes insulin, which is a hormone that helps glucose get into your cells to be used for energy. But when your body doesn’t make enough—or any—insulin (Type 1 diabetes), or doesn’t use insulin well (Type 2 diabetes), then glucose then stays in your blood and can cause health problems.
In November 2020, a global analysis published in the journal Diabetes, Obesity and Metabolism found that up to 14.4% of people who were hospitalized with severe COVID-19 also developed diabetes. But why?
- Long Covid damages the brain. You can develop all of the symptoms below. You can develop mental health problems and even psychosis. Finally, it fucks with your senses.
Here is another EXCELLENT diary that explains how COVID attacks the brain. If you want to know more, go over there and rec and read it.
COVID Reduces Grey Matter in Areas of the Brain Related to Memory & Executive Function
There are many ways that COVID-19 can damage the brain. As I described in a previous blog post, some can be devastating, such as encephalitis, strokes, and lack of oxygen to the brain. But other effects may be more subtle, such as the persistent impairment in sustained attention noted by Chinese researchers.
In addition to direct effects on the brain, COVID-19 can also have long-term effects on other organ systems. So-called long haulers can have other lingering symptoms including fatigue, body aches, inability to exercise, headache, and difficulty sleeping. Some of these problems may be due to permanent damage to their lungs, heart, kidneys, or other organs. Damage to these organs — or even just the symptoms by themselves — can impair thinking and memory and cause brain fog. For example, how can you think clearly if you’re feeling fatigued and your body is aching? How can you concentrate if you were up half the night and awoke with a headache?
Here's why that is a HUGE deal.
- Long Covid attacks the nervous system. It causes small fibers to misfire and causes a low level of background pain and then migrating intense pain, usually starting in the feet and then moving throughout the body. This is what I suspect I have instead of fibromyalgia.
Long Covid and Covid attack the reproductive system of both males and females. It also attacks the placenta which can kill the fetus and lead to a very traumatic and painful stillbirth.
Stillbirths: COVID Can Severely Damage the Placenta
Research published Thursday paints a startling picture of the destructive toll Covid-19 can take on pregnant women and their growing fetuses.
The virus can attack and destroy the placenta, a vascular organ that serves as a fetus’s lifeline, leading to asphyxiation and stillbirth, according to the study in the journal Archives of Pathology & Laboratory Medicine.
“We have never seen this level of destruction from an infectious illness before. It rendered the placenta unfit to carry out its duties,” said Dr. David Schwartz, a perinatal pathologist in private practice in Atlanta, who led the study. “These fetuses and newborns died from asphyxiation due to lack of oxygen.”
Grim indeed. Now, not everyone gets the worst effects of COVID above. However, 30-40% of people have reported some type of Long Covid. The relapse rate for post-polio is about 1-2%. What could it be for COVID 40 years down the line? Sobering thought.
The GOOD News: research on Long Covid may figure out how the immune system works
It may find cures for all autoimmune diseases and chronic illnesses.
Long Covid, because it is so prevalent, means researchers can cast a wider net.
There are almost as many questions about long Covid as there are symptoms. From the pandemic’s early days, a significant share of people have been troubled by problems that persist for weeks or even years after their acute infection clears, or find they’ve developed new issues that range from bothersome to debilitating. These difficulties span the mind and the body, and so far they resist explanation.
Current treatments focus on easing brain fog, bone-wearying fatigue, shortness of breath, muscle pain, loss of smell, anxiety and depression, and sleep problems, but two burning questions remain unanswered: Who gets long Covid and how can it be prevented?
On Monday, a consortium of six Boston hospitals (Beth Israel Deaconess Medical Center, Boston Medical Center, Brigham and Women’s Hospital, Cambridge Health Alliance, Massachusetts General Hospital, and Tufts Medical Center) joined RECOVER, a national, 15-member effort sponsored by the National Institutes of Health whose mission is to understand, prevent, and treat long Covid, which it calls post acute sequelae of SARS-CoV-2 infection, or PASC.
It seems there are 4 (so far) main risk factors that set you apart for a severe infection and long COVID:
A new studyTrusted Source noted that post-acute sequelae of COVID-19, also known as PACS, represent an “emerging global crisis.”
In the study, researchers identified four factors in people that appear to be linked to an increased risk of having long COVID:
- type 2 diabetes
- the reactivation of Epstein-Barr, a virus that is present in most people but remains dormant in many
- the level of coronavirus RNA in the blood early in the infection, an indicator of viral load
- the presence of certain autoantibodies, which mistakenly attack tissues in the body as they do in autoimmune diseases such as lupus and rheumatoid arthritis
Scientists are trying to figure out why some people seemingly cannot be infected.
Scientists Seek to Find Out Why Some Cannot Seem to Catch COVID
Phoebe Garrett has attended university lectures without catching Covid; she even hosted a party where everyone subsequently tested positive except her. “I think I’ve knowingly been exposed about four times,” the 22-year-old from High Wycombe said.
In March 2021, she participated in the world’s first Covid-19 challenge trial, which involved dripping live virus into her nose and pegging her nostrils shut for several hours, in a deliberate effort to infect her. Still her body resisted.
“We had multiple rounds of tests, and different methods of testing: throat swabs, nose swabs, other types of swabs that I’d never done before like nasal wicks – where you hold a swab in your nose for a minute – as well as blood tests, but I never developed symptoms, never tested positive,” Garrett said. “My mum has always said that our family never gets flu, and I’ve wondered if there’s maybe something behind that.”
Scientists think they are getting close, but it may need a few more years of dedicated research.
zmom has shared a study about long haulers seeing improvements in chronic fatigue after using a hyperbaric oxygen chamber.
Background: Long COVID is a common occurrence following COVID-19 infection. The most common symptom reported is fatigue. Limited interventional treatment options exist. We report the first evaluation of hyperbaric oxygen therapy (HBOT) for long COVID treatment.
Methods: A total of 10 consecutive patients received 10 sessions of HBOT to 2.4 atmospheres over 12 days. Each treatment session lasted 105 minutes, consisting of three 30-minute exposures to 100% oxygen, interspersed with 5-minute air breaks. Validated fatigue and cognitive scoring assessments were performed at day 1 and 10. Statistical analysis was with Wilcoxon signed-rank testing reported alongside effect sizes.
Results: HBOT yielded a statistically significant improvement in the Chalder fatigue scale (p=0.0059; d=1.75 (very large)), global cognition (p=0.0137; d=-1.07 (large)), executive function (p=0.0039; d=-1.06 (large)), attention (p=0.0020; d=-1.2 (very large)), information processing (p=0.0059; d=-1.25 (very large)) and verbal function (p=0.0098; d=-0.92 (large)).
Conclusion: Long COVID-related fatigue can be debilitating, and may affect young people who were previously in economic employment. The results presented here suggest potential benefits of HBOT, with statistically significant results following 10 sessions.
Conclusion: My Personal Hell
My maiden diary was written about fifteen months ago now. It was written in response to people hesitating to get the vaccine to show them what long hauling life was like.
Since then, I have had until this day:
1) Unendurable pain while working in the home remodeling business. There was a background level of pain and then severe pain in one or more joints. It got to the point where I could barely walk and my arms could barely move. I have pulled two different muscle groups (calf and scapular). I have been diagnosed with fibromyalgia and I attended intense physical therapy. The combination of drugs and physical therapy means I am almost fully mobile again.
2) Doing the worst of Covid I lost about 30 pounds. Due to changes in my metabolism and a suspected fatty liver, I have gained back about 50 pounds. I am very obese, and that increases the fibromyalgia pain even further. I have to see a nutritionist to go on a strict diet that is mental health and fibromyalgia friendly. Oh, and I need to exercise more even though that hurts like an MFer.
3) I have had a severe mental breakdown once again. This time, it was severe enough to spend time in the psych ward for a week. I am about six weeks removed from that experience, and I never want to live that again. However, the two drugs I was on have created another manic phase, so I am greatly concerned I will never find a correct balance.
4) A combination of fragile lungs and obesity means I have great difficulty breathing at times. At night I have to use a CPAP machine. I now have a rescue inhaler just in case too much walking or moving or working the limited amount I do causes me to suffer when I have difficulty breathing.
5) My heart beats fast randomly and my blood pressure spikes for no discernible reason. I have had to visit urgent care 2-3 times to have them do the vagal maneuver on me to reset my rhythm. It’s lucky I haven’t had a heart attack or stroke.
6) My kidneys… work.. funky. They still function as far as doctors can tell, but there have been issues with UTIs and other issues.
7) My immature white blood cell count is abnormally high, while the specialized count (like T cells) are low. This is usually a sign that there is an autoimmune response to an infection. Long Covid likely causes an autoimmune disorder.
8) On some days, my brain fog can be intolerable. I have to make sure when I am lucid to write everything I need to do down multiple times and in multiple places. I have 15 reminders active on my phone just for doctor appointments. The other chore based things I have on an Autism Spectrum Disorder chart just like I would have used in teaching. It prompts me when I forget what to do next.
9) I try not to think about it, but I wonder what this virus does to the body 20, 30, and 50 years down the line. Will it be like shingles or post-polio? What is my life expectancy (especially with bipolar)? How am I going to pay all of my bills? How will I find work that is within my many restrictions?
To summarize this diary, I leave you with this thought:
You don’t want to let your guard down. You are still playing Russian roulette with three chambers full. And we all know how awesome something Russian is right now...
Wednesday, Mar 9, 2022 · 2:58:59 PM +00:00 · bilboteach
Have people asking about a possible 4th vaccine dose. Here are some articles and research and opinions about this happening.
Will We Need a 4th Dose? (bolded emphasis mine)
Research shows that a booster or third dose of an mRNA COVID-19 vaccine provides greater protection against infection from Omicron. However, some evidence suggests that booster protection wanes by about 15% to 25% after 10 weeks. Does this mean we’ll need a fourth vaccine dose sometime soon?
Currently, there’s not enough evidence to support the need for a second booster shot among non-immunocompromised individuals. The Centers for Disease Control and Prevention (CDC) only recommends that people with weakened immune systems get a booster shot on top of their three primary doses.
However,
On Friday, Feb. 11, 2022, the CDC published a study showing that both Pfizer and Moderna’s booster shots lost substantial effectiveness after four months during the Omicron surge.
Researchers found that boosters were highly effective against severe and moderate illness for about two months after an initial vaccine series. But once the fourth-month mark hit, that effectiveness significantly declined. The study said this suggests the need for additional boosters in the future.
During those first two months post-booster, the vaccine was 91% effective at preventing hospitalization. But after four months, that dropped to 78%.
Vaccines were also less effective at preventing emergency department and urgent care visits during the Omicron period. Booster protection went from 87% in the first two months to 66% after four months. After five months that number fell to 31%. However, researchers say that the latter number is “imprecise” because there was little data on people who’d received a booster five months prior.
The FDA is looking into research on the second booster shot:
U.S. health regulators are looking at authorizing a potential fourth dose of a COVID-19 vaccine in the fall, the Wall Street Journal reported on Saturday, citing sources familiar with the matter.
The Food and Drug Administration has been reviewing data to authorize a second booster dose of the messenger RNA vaccines from Pfizer Inc and partner BioNTech SE and vaccines from Moderna Inc, the report added.
The FDA did not immediately respond to a request for comment.
The agency last month cut the interval to get a booster dose of COVID-19 vaccines from Pfizer and BioNTech as well as from Moderna, in a bid to provide better protection sooner against the Omicron variant.
Wednesday, Mar 9, 2022 · 3:30:35 PM +00:00 · bilboteach
As for an Omicron specific booster, it looks like research in this specific area hit a dead end.
Omicron Booster No Better Than Regular Booster
In a small group of monkeys, an omicron-specific version of Moderna's COVID-19 vaccine did not protect against the omicron variant better than Moderna's current, highly effective booster. This finding casts doubt on whether a switch to variant-specific doses is necessary.
The study was led by researchers at the National Institutes of Health and posted on a preprint server last Friday. The study has not been peer-reviewed or published in a scientific journal. It also has all the limitations of an animal study and only involved eight monkeys. The study's findings will have to be verified in human trials, which are currently underway.
Still, there's good reason to think the finding will hold up. As the authors of the study note, this isn't Moderna's first variant-specific booster. The company had previously developed a booster against the concerning variant beta. As with the omicron-specific booster, the beta-booster didn't outperform the original vaccine at protecting primates from beta. And that finding later held up in human trials.
Wednesday, Mar 9, 2022 · 5:31:55 PM +00:00 · bilboteach
scooba writes deep in the comment section that COVID can have a terrible effect on your eyes and your teeth. The only place I haven’t looked at is the stomach. I bet it does a number on it too!
Also, I’ve never been at the top of the rec list before. Honored. Never been happier to be proven wrong (I wrote a comment that no one will read or see this).
Wednesday, Mar 9, 2022 · 6:32:00 PM +00:00 · bilboteach
I didn’t talk about the digestive system, but a quick search shows that the digestive system isn’t untouched by COVID either.
Covid Attacks the Gut Microbiome
A reduction in bacterial diversity in the gut microbiome was noted in 41% of the healthcare workers and 65% of the elderly COVID-19 patients as compared to the 25% diversity loss observed in the reference sample. Stool samples of around 2% of the healthcare workers and 61% of the COVID-19 patients tested positive for SARS-CoV-2. Notably, stool samples of seven out of the eight patients who died during COVID-19 hospitalization tested positive for SARS-CoV-2.
Remember, there is a link between depression/mental illness and the gut microbiome that is just beginning to be understood.
Covid Can Trigger Multiple Symptoms in the Digestive System
The first person with confirmed COVID-19 in the United States experienced 2 days of nausea and vomiting before developing diarrhea. And one of the earliest American studies found that around 32% of patients with the disease reported GI symptoms, most commonly diarrhea, nausea, or a loss of appetite.
The research is ever-evolving. According to a February 2021 reviewTrusted Source that included 125 articles and a total of 25,252 participants, the most common GI symptoms of COVID-19 included:
- lack of appetite (19.9%)
- distortion or lack of taste (15.4%)
- diarrhea (13.2%)
- nausea (10.3%)
- vomiting up blood or GI bleeding (9.1%)
Other than lack of taste, it seems that none of these symptoms are long term. But more research likely needs to be done.
Thursday, Mar 10, 2022 · 6:34:48 AM +00:00 · bilboteach
Yet more organs and body systems that COVID can attack and leave lasting damage to:
Long COVID can attack your thyroid. It does so by inflaming the tissue and subtly changing the hormones produced by the gland. The thyroid plays a key role in metabolism and many other key functions.
Yet another organ seems to be affected by a bout of COVID-19: the thyroid.
Italian researchers have examined the thyroids of dozens of patients who've recovered from moderate-to-severe cases of COVID-19. The study found evidence that SARS-CoV-2 infection may trigger an inflammation of the gland in some patients.
Whether that inflammation can cause long-term dysfunction is still unclear, however.
"After three months, patients' thyroid function has normalized, but signs of inflammation were still present in about one-third of patients," study lead researcher Dr. Ilaria Muller, of the University of Milan, said in a news release from The Endocrine Society. Her team presented their findings Monday at the virtual annual meeting of The Endocrine Society.
As for the parathyroid, there is evidence that COVID damages it as well, but the organ has been little studied in regards to COVID or Long Covid.
We read with great interest the research article of Liu et al. who found that almost two third of patients with novel coronavirus disease (COVID-19) had hypocalcaemia [1]. Few mechanisms which explain the causes of hypocalcaemia in COVID-19 have been discussed, such as vitamin D deficiency, hypoalbuminemia, impaired intestinal absorption of calcium, hypoxic tissue damage with subsequent increase in calcium influx and impaired secretion of and response to parathyroid hormone (PTH) secondary to increased levels of inflammatory cytokines [1]. We would like to add another two possible mechanisms which discuss the possible effects of COVID-19 on parathyroid glands that could improve our understanding of the possible link between this disease and hypocalcaemia.
To date, little is known about the effect of the novel coronavirus (SARS-CoV-2) on parathyroid glands…
Beyond swollen lymph nodes, I cannot find any definitive answer for what COVID does to the lymphatic system. Too much of the zone has been flooded with “swollen lymph nodes due to the vaccine”, especially on vaccine misinformation sites.
As for the gallbladder, in some cases a highly lethal complication can develop months after release from the hospital. Thankfully, this complication seems rare.
A new horrific post-COVID condition has been reported from the Indian capital Delhi, with at least five people who have recovered from the deadly virus contracting gallbladder gangrene. The condition has a high morbidity rate and the patients required emergency surgery, doctors at the Sir Ganga Ram hospital said.
The hospital said five recovered Covid patients — four men and a woman, ages between 37 and 75 — returned in the past two months, and four of them had holes in their gall bladder.
COVID also fucks with adrenal gland function. This is thought to be one of the keys behind Long Covid occurring, but scientists are not 100% sure yet. The adrenal gland is one of the most critical glands in your body.
Finally, some studies have addressed the concern of adrenal insufficiency during the long-term recovery phase. Dr Sara Bedrose, adrenal endocrine specialist at Baylor College of Medicine, indicates that studies which included adrenal function in COVID survivors showed a large percentage of patients with suboptimal cortisol secretion during what is called ACTH stimulation testing.
Results indicated that most of those cases had central adrenal insufficiency. It was concluded that adrenal insufficiency might be among the long-term consequences of COVID-19 and it seemed to be secondary to pituitary gland inflammation (called hypophysitis) or due to direct hypothalamic damage. Long-term follow-up of COVID 19 survivors will be necessary to exclude a gradual and late-onset adrenal insufficiency.
Some patients who have COVID-19 will experience prolonged symptoms. To understand what is happening to them, patients may question whether or not they have a phenomenon called adrenal fatigue. This is a natural question to ask, especially after having such a severe health condition. A tremendous amount of resources are being developed to investigate the source and treatment of the symptoms, and this work has only just begun.
It even attacks the pituitary gland, which is like the master switch for the whole system of hormones inside your body.
Hypothalamus-pituitary, aka ‘the master gland‘
“Nicknamed ‘the master gland,’ the hypothalamus-pituitary are responsible for sending signals to all other glands of the endocrine system. When those signals are not secreted properly those glands stop producing the hormones they are designed to secrete.”
In terms of a patient with COVID-19? It’s difficult to tell if a disrupted hypothalamus-pituitary is a COVID-specific effect or the result of another illness.
Thursday, Mar 10, 2022 · 8:02:51 AM +00:00 · bilboteach
Here is another EXCELLENT compilation of interesting Long COVID articles, particularly showing the increased deterioration of the brain. And it appears the virus may lay dormant in the body.
It lines up neatly with the diary novapsyche posted yesterday as well.


