There's been a lot of discussion about the Senate bill, but I haven't seen many diaries that detail the cost controls contained in the bill. I have, however, seen many comments by people saying that there are no cost controls in the Senate bill. This is either misinformation or a misunderstanding and my goal this afternoon is to set the record straight and explain the cost controls that are in the Senate HCR bill.
I have an additional goal this afternoon - and that is to explain what we need to do next. We need to get to work quickly to make sure that the good that's in this bill stays there and that the bad that can be improved, gets improved. Now, we're not going to be able to do much about Nelson's ridiculous abortion amendment, but there are actions we can take to limit the damage. We're not going to be able to put a public option back in during conference, but there are things we can do that will change the bill in a good way that won't trigger the Nelson/Lieberman filibuster of the final conferenced bill.
So, let's get started!
Cost Savings
Johnathan Cohn tackles cost and explains how the Senate bill will keep costs lower for consumers. There's an important chart here - if you haven't seen it, here's a link.

Looking at this chart, it's easy to see how premiums are cheaper for consumers if this bill does pass. Without the bill, premium costs will remain ridiculously high and insurance coverage (and therefore health care) will still remain be out of reach for many.
The Kaiser Family Foundation has a Subsidy Calculator that you can use to see if you would qualify for help with your premiums. If you make between 133% and 400% of the Federal Poverty Level you will qualify for subsidies. If you make less than 133% you qualify for Medicaid.
Cohn put together some important charts for you to see what the cost of no reform would be:
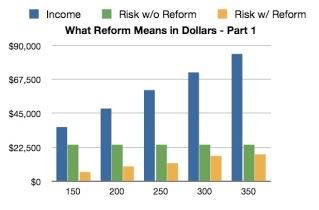
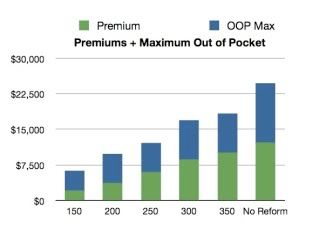
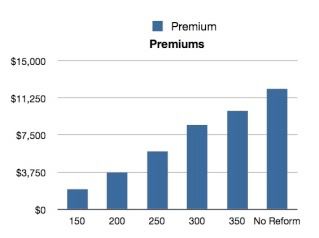
Would the Senate bill limit costs as much as we would prefer? No. Frankly, if we're talking about preference, I'd "prefer" we have a single payer program. We don't have the votes for what we'd prefer, but we do have the votes for for this bill and I think the cost savings are pretty clear if the option is this or nothing at all.
Cost Controls
As for actual "cost controls" in the bill. A lot of people have suggested that they aren't there. This just isn't true. There are a large number of cost controls in the bill. Here's a good list and a description of each:
Premium Increases? One argument that a lot of people have put forward is that health insurance plans can automatically start increasing premiums - and that there's somehow no ceiling to premium increases. Ezra Klein helps debunk this:
Under health-care reform, there are at least three bulwarks against the monopoly-profits scenario: Inter-insurer competition, regulators, and the tax on excessive premiums. Two of these mechanisms don't exist in the current market. One -- the market itself -- is much weaker and more opaque, and individuals have a far harder time navigating it. Link.
- If my insurer on the exchange increases cost I can switch to one that is cheaper.
- If my insurer tries to increase premiums beyond a reasonable amount, the exchange will kick them out. Link.
- If they raise premiums too high then they are required to pay a 40% tax on the plan that they're offering (the excise tax).
All three of these regulations work together to limit the likelihood that any insurer will increase their premiums exorbitantly.
Bundled Payments & quality of care
As always, Ezra Klein has the explanation.
Under bundled payments, the hospital would receive one check for everything related to your stroke over a single period of time. That means they make more money from doing less, rather than more money from doing more. It also gives them an incentive to coordinate care when you're out of the hospital, as it's cheaper to get a nurse to call and make sure you're taking your medicine than it is to have you in for a follow-up procedure.
This relates to Medicare in a big way. One of the aspects of the bill - and one of the ways we're paying for hcr is through cost savings in Medicare. Medicare Part A pays for hospital coverage. As we sit right now Medicare Part A spends approximately $17 billion on hospital readmissions each year. Why are these people being readmitted for the same issue?? Because the hospitals are discharging them early and/or not providing them with a good quality of care and with instructions on how to follow up once they leave. There's no disincentive for hospitals to discharge early at this point. Sure, people can file quality of care complaints, but that hasn't stopped hospitals from using this practice. Medicare can save $17 billion if hospitals use bundled payments and have quality of care requirements.
More info on quality of care reporting can be found here - follow the links if you're interested. One of the reasons health insurance costs are so high is that health care is expensive. If health care providers and hospitals are reporting on quality of care there is incentive to provide better care - better care will lower costs over time which will help control insurance costs. Another thing that will help, pricing transparency.
Transparency
As I mentioned before, if an insurer tries to increase premiums beyond a reasonable amount, the exchange will kick them out. Link. But in addition to that, the companies participating in the exchange will be required to report quite a bit of data, including the percentage of claims denied. When you're shopping around on the exchange, you will have access to all of this data. This is similar to how Medicare Advantage plans and Prescription drug plans are required to report back to CMS. You can see how this data is compiled on all the plans on Medicare.gov if you go to the section on comparing prescription drug plans. I'm sure some of you are familiar with this.
Mandates
Let me start by saying that I don't like mandates. I've never liked mandates. When the primary was happening one of the reasons I preferred Obama to the other candidates was that he said he didn't support mandates. Let me also say that I am willing to compromise my complete hatred for mandates so that we can get a health care reform bill.
There are good arguments for and against mandates. We've read some of those here and some in other places. The argument is that mandates will help keep costs low.
First, the individual mandate lowers average premium costs by bringing healthy people into the system. If the only people buying insurance are the people who expect to need to use it, the average cost will be prohibitively high. But second, the individual mandate is the political spur for future cost controls. Link.
I understand this argument. I can see that costs have come down in MA where they have mandates. I still don't like them. Anyway, my favorite health care blogger, Ezra Klein (he's cute too!) responds to some of the criticisms of mandates here.
Pilot Programs
Atul Gawande talks about how pilot programs will help save money in the long run. It's a good article.
Mark Warner and 9 other freshman Democrats introduced the Value and Innovation Package, which is where you can find a few of the pilot programs. There are some great cost-saving programs here for both Medicare and Medicaid.
Here's one of them:
Sec. 3602. Pilot Testing Pay-for-Performance Program for Certain Medicare Providers.This section would direct the Secretary to begin pilot testing of value-based purchasing (pay-for-performance) programs for certain types of Medicare providers no later than January 1, 2016. These provider types include: inpatient psychiatric hospitals, long-term care hospitals, inpatient rehab facilities, acute prospective payment system-exempt cancer hospitals, and hospices. The Secretary would have authority, after 2018, to expand these pilots if the CMS Chief Actuary determines it would reduce Medicare program spending while maintaining or improving the quality of care.
Another element here is state innovation. And again, I give you Ezra Klein(are you sick of him yet? I'm not. ):
In a bill that tries to think of everything, there’s a provision that tries to think of that, too. Section 1332, to be exact.
Section 1332 is titled "Waivers for State Innovation." But that’s a terrible name. Call it "the law for the law of unintended consequences." The idea is simple: If states think they can do better than the language and policies in this bill, and they can make a convincing case that they’re right, they can get a waiver exempting them from the legislation. They still get the money that would be owed to them, but they get to spend it their way. Link.
This allows states to come up with their own plans. Basically, if the state of Rhode Island wants to allow everyone access to the exchange, they can. If they want to develop their own single payer plan, they can. If one state has a successful innovation, it is likely that other states will begin to adopt those ideas and those savings.
Medical Loss Ratio
Under the proposal by Senate Democratic leader Harry Reid, health insurance plans for large groups would have to spend at least 85 cents out of every dollar on medical costs. That means just 15 cents could go toward overhead and executive salaries, among other things. Small groups or individual plans would have to spend at least 80 cents on the dollar for care. Link.
At the moment, the average private insurance industry has a 30% MLR. This bill would force them to cut that in half (depending on where they stand with regard to the average). Some states currently allow MLR's up to 40 and 50%. I've seen several people suggest that this will result in premium increases so that they can "make up the difference" by adding more dollars to the pot. Unfortunately, that won't work for several reasons.
- In order to increase premiums they would have to increase medical services offered. This could put them at risk for the 40% excise tax if the plan and coverage becomes ridiculously expensive.
- Increasing their premiums unfairly could get them kicked out of the exchange (as I stated above) and as a result they could lose a lot of business.
- If they increase the premiums and don't meet the MLR required, they have to refund the difference to the consumer - so either way, they pay.
Some of the other cost controls in the bill are expanded on by (again) Ezra Klein, here. One of these is "prudent purchasing", which I believe I've already covered.
Prudent purchasing means that insurers can't enter, or stay, in the exchanges unless regulators are satisfied that they're doing a good job.
Basically, OPM is going to manage and regulate these exchanges, so if insurers do a poor job, they won't be able to participate. This is good news, but it also means that we need to continue to work hard to elect Democrats so we can stay in charge.
I've heard this argument a lot: But there's no public option...so there's not enough competition and that won't really control costs.
Jacob Hacker, the man known as the Godfather of the Public Option, has a response:
The public option was always a means to an end: real competition for insurers, an alternative for consumers to existing private plans that does not deny needed care or shift risks onto the vulnerable, the ability to provide affordable coverage over time. I thought it was the best means within our political grasp. It lay just beyond that grasp. Yet its demise -- in this round -- does not diminish the immediate necessity of those larger aims. And even without the public option, the bill that Congress passes and the President signs could move us substantially toward those goals. Link.
I thought it would be useful to look at what Politifact has to report on Obama's progress with regard to his campaign promises. I encourage you to go through this list because you will find that many of these promises are also in the "cost controls" category and they are part of the Senate bill.
An example:
Close the "donut hole" in Medicare prescription drug plan:
"Barack Obama wants to close the 'doughnut hole' in the Medicare Part D Prescription Drug Program that limits benefits for seniors with more than $2,250 but less than $5,100 in annual drug costs. Approximately 4 million seniors hit the doughnut hole in 2006, paying full price for drugs while also paying drug plan premiums."
Millions of Senior who currently hit that donut hole and stop taking their medications will be able to afford their drugs as we fill in the donut hole over the next few years. This won't just save money for Seniors, it will also save money for Medicare. Currently, many Seniors stop taking their medications and then end up in the hospital with serious complications, heart attack, etc. which only ends up costing those Seniors and Medicare more money in the long run.
If you're interested, I recommend comparing the Senate bill to the campaign health care plan. Most of what is in the campaign plan is in this Senate bill. President Obama is saying today in the WaPo that everything he campaigned on is in the HCR bill. He may be right if you look at the list. Of course, there's also some anti-choice garbage that made it in there. Here's a good summary of what's changed recentlyin the Senate bill (Ezra again).
Now...finally...What do we do next??
First, the Nelson amendment pisses me off. I don't see how we'll be able to kill it and still get votes, but I do know what we can do to help the situation while we work on getting Congress to repeal this amendment.
- Donate to Lilith Fund
- Donate to Planned Parenthood
The women who will mostly be impacted by this amendment most likely can't afford abortions now and they will likely be unable to get insurance coverage for abortions (depending on the state). This isn't a new problem. It's an ongoing problem. So, to help fix it. Please donate to these organizations which help women in need pay for abortions that they need.
Second step to take is to contact your House Rep AND your Senator. Tell them that you want the preexisting conditions clause to take effect immediately for everyone, not just children. We need this to start in 2010 for everyone and the Senate bill only ends preexisting conditions for children in 2010.
Don't stop there. You also need to bring up the start date for the exchange. The Senate bill starts the exchange in 2014. If we can move that up by even a year that would be better than what it is now. Senator Harkin is already suggesting this, so let's make calls and push for it.
Update: Please visit tunesmith's diary, What To Improve In Conference for more suggestions.
Find your Senators here. Find your House Reps here.
Get on the phones. Please consider a donation if you can afford to help. Let's work to improve this bill. We only have a few weeks before the final vote.


