Everything we’ve been hearing concerning the complaints with Obamacare either involve rising prices or lower choices due to only a lower insurer participation within the exchanges. We’re told that the solution to this problem is to “give states more power” and to “give states more flexibility” instead of having this “one size fits all” system.
When people say that they are ignoring basic facts and reality. They’re ignoring the very real phenomenon of political sabotage.
When it came to control prices and costs with the ACA, all that power wasn’t under the control of the federal government — all that power was always intended to be delegated to the states.
Health insurance premiums have risen rapidly, straining pocketbooks for American families and businesses. Since 1999, the health insurance premiums for family coverage have risen 131 percent. Premium increases have forced families to spend more money for less coverage. And insurance companies have been able to raise rates without explaining their actions or justifying the reasons for their high premiums.
The Affordable Care Act brings an unprecedented level of scrutiny and transparency to health insurance rate increases. Thanks to the Affordable Care Act’s requirement that insurance companies publicly justify any unreasonable rate increases, consumers who experience large increases will know why they are paying the rates that they are. On December 21, 2010, the Department of Health and Human Services, working in partnership with states, proposed a new regulation to implement this important consumer protection.
That was the plan, the question is “how well did it work?” Well, when you have several states that are controlled by partisans who are more interested in grinding axes rather than helping their constituents, not always that well.
The Highlight Talking Points or Dems are as follows:
- Waiver options already exist in Obamacare but only 8 States have used them.
- ObamaCare allows State Insurance Commissioners to control rates, some of them haven’t bothered.
- Only half the States Implemented their own ObamaCare exchange, those that didn’t have less control off their market and have higher premiums.
- Many states that didn’t expand Medicaid also have more premium restrictions as their poorest have to use unpaid emergency services that generally increase prices.
- States without Insurance Reforms, their own Exchanges and that didn’t expand Medicaid generally have 11% higher premiums than those states that did.
Just to clear up something about Graham-Cassidy there is first and foremost the argument over it’s coverage of pre-existing conditions. In this segment Rick Santorum claims that he himself wrote the pre-existing condition portion of the bill, and he claims that states are only granted a waiver if they can ensure that their alternative is “adequate and affordable” based on the opinion of the HHS secretary.
1.Waiver options already exist in Obamacare but only 8 States have used them.
What people like Santorum ignore is that there are already options available for states to “experiment” under the affordable care act by using it’s innovation waiver program.
Section 1332 of the ACA allows states, beginning in 2017, to modify key parts of the health law in service of state-specific strategies to improve coverage. States that pass legislation authorizing an innovation waiver can apply to the federal government to waive rules concerning essential health benefits, the law’s premium and cost-sharing subsidies, the marketplaces, and the individual and employer mandates, among others. (Some protections aren’t waivable. These include the ACA’s nondiscrimination rules, protections for people with preexisting conditions, and prohibitions on health status and gender rating.)
State flexibility to change the ACA is significant, but it isn’t unlimited. Federal law makes clear a waiver can’t be granted unless the state demonstrates its proposal meets four conditions. Coverage under the waiver must be at least as 1) comprehensive and 2) affordable as without it, 3) cover a comparable number of residents, and 4) not add to the federal deficit. The Obama administration explained that these legal limitations require federal officials to consider both the overall impact of a waiver on state residents and any disparate effects a proposal may have on vulnerable populations, including those with low incomes, older Americans, and those with serious health issues.
 State that have drafted, submitted and implement ACA Waivers
State that have drafted, submitted and implement ACA Waivers
And there many other provisions within the existing ACA that give states latitude and power as long as they maintain current coverage levels and pricing. At this point in time only 15 states have even bothered to even draft a set of waivers, 5 are under under Federal Review, 2 have been approved without being implemented and only 8 states have completed the process with their own legislation.
Conservatives keep saying the states are “clamoring” for this flexibility, but the truth is they already have it and aren’t doing all that much with it.
2. ObamaCare allows State Insurance Commissioners to control rates, some of them haven’t bothered.
The “great laboratory of the states” is in fact, already in place. It has been for some time starting with the power of the states to review all proposed rate increase by insurers in their jurisdiction. The Rate Review process was a new feature introduced by the Affordable Care Act that many people don’t realize exists and don’t realize is controlled by local State Insurance Commissioners.
The Affordable Care Act (ACA) requires that insurers planning to significantly increase plan premiums submit their rates to either the state or federal government for review. The threshold for this requirement is 10%.
The rate review process is designed to improve insurer accountability and transparency. It ensures that experts evaluate whether the proposed rate increases are based on reasonable cost assumptions and solid evidence and gives consumers the chance to comment on proposed increases.
The ACA also requires that a summary of rate review justifications and results be accessible to the public in an easily understandable format.
Any insurer that submits an increase of 10% or more has to have that increased reviewed and approved By. The. State.
Compared to price increases of 131% since 1999, price increases since 2010 have gone down substantially, but still more needs to be done.
The recent debate on health care reform has occurred mostly at the national level. The Affordable Care Act, or ACA, was a momentous change for the American health care system. So far, 20 million people have gained health insurance coverage due to the ACA — a historic reduction in the number of uninsured people in the United States.
…
Partly due to the ACA, health care cost spending growth has slowed in recent years. Before 2014, there were five years of historically low growth, and 2011 was the first time in a decade that spending on health care grew more slowly than the U.S. economy. Health care costs are still projected to grow faster than the overall economy, however, and health care spending already puts tremendous pressure on state and federal budgets and limits spending on other important services. More needs to be done to sustain this slowdown in growth.
When those who criticize Obamacare say rates are rising sharply in some states, they almost always neglected to mention that many of these increases are because cuts to the Cost Sharing Rate (CSR) payments which the Trump administration has been threatening to withhold, as a result driving costs for individuals up and that local states insurance commissioners are those who have consequently approved those rate increases.
In Mississippi, for example, the insurance commissioner approved a 47.4% average rate increase for the state’s single Affordable Care Act exchange insurer, The Wall Street Journal reports. The increase would have been just 17.9% if CSR payments were guaranteed next year.
Connecticut approved a 31.7% premium increase for Anthem and a 27.7% increase for ConnectiCare, the article adds, and Kentucky, Mississippi and Virginia all are approving rates for major insurers that are at least 25% higher than rates were this year.
In Illinois, state regulators submitted rates to the federal government that would increase the average cost of the lowest-priced silver plans by 35%, the Chicago Tribune reports. The lowest-priced bronze plans in the state will see an average 20% rate hike, while premiums for the lowest-priced gold plan will increase 16% on average.
Premium tax credits, which increase when premiums go up, will shield many ACA exchange customers from such steep increases, but not all enrollees qualify for those subsidies.
The mechanism already exists to help control high prices increases, but only if that particular state fully implemented the ACA suggested price reforms. Not all of them did..
3. Only half the States Implemented their own ObamaCare exchange, those that didn’t have less control off their market and have higher premiums.
Even though it’s hardly ever mentioned any more than two dozen states refused to even implement their own state based exchanged as the original ACA intended, this was not supposed be a massive “single solution” but one that would allow each state to tailor things to their state.
In the end this is how it broke down with the Exchanges.
 State Based and National Exchanges
State Based and National Exchanges
Those states that refused to create their own exchange generally charged higher premiums as a surcharge for the Federal Government setting up an exchange for them.
Residents of states that refuse to set up health insurance exchanges under Obamacare are set to be hit with higher premiums under new rules announced by the Health and Human Services Department. Insurance companies will be charged 3.5 percent of any premiums they sell through the federal exchanges, the department announced Friday.
And insurers are likely to pass that surcharge on to clients, leading to higher premiums. The only states to be affected are those that refuse to set up their own exchanges because of opposition to the Patient Protection and Affordable Care Act. They are almost certain to be those under Republican control. In those states, HHS will set up the exchanges
So those who didn’t setup exchanges were already working at a disadvantage.
4. Many states that didn’t expand Medicaid also have more premium restrictions as their poorest have to use unpaid emergency services.
This made even worse by states that chose not to accept the ACA Medicaid expansion which would ease the general burden on everyone else by forcing those people into our emergency rooms.
 State by Sate Medicaid Expansion
State by Sate Medicaid Expansion
Notice anything familiar? Most states that didn’t implement their own exchanges, also didn’t implement the Medicaid expansion. Exceptions include Idaho, Utah and Mississippi who all did have their own exchanges but still didn’t expand Medicaid. Similarly Idaho, Missouri, Iowa, Indiana, Ohio, Wisconsin, North Carolina and Mississippi also didn’t implement the insurance reforms which would have given their state commissioner more power to block excessive price increases.
5. States without Insurance Reforms, their own Exchanges and that didn’t expand Medicaid generally have 11% higher premiums than those states that did.
When you look at recent price increases, they also follow the same similar pattern on the map. [Note some states have actually had their insurance premiums decrease this year as shown in yellow — particularly Arkansas which implemented waivers, insurance reforms, setup a partnered exchange and also expanded Medicaid, and Washington which has an exchange, reforms and the Medicaid expansion.]
 County by County look at price increase for 2017
County by County look at price increase for 2017
Here they are broken down state by state as noted by our own Charles Gabs.
 State by State rate changes
State by State rate changes
- 2017 premium increases emerged A private non-profit web service by Charles Gaba posts a comprehensive tracker of rate filings including projected overall, weighted average rate changes for the individual market. Kaiser Family Foundation has an examination of 2017 premium changes and issuer participation. It is presented with the following statement, " in general, 23% seems to be the number to look at for requested increases overall." During September and October it was up to state regulators to either approve or change those requests.”
Specifically Gaba has pointed out that the average weighted increase for ACA compliant states is 11% lower than non-compliant states.
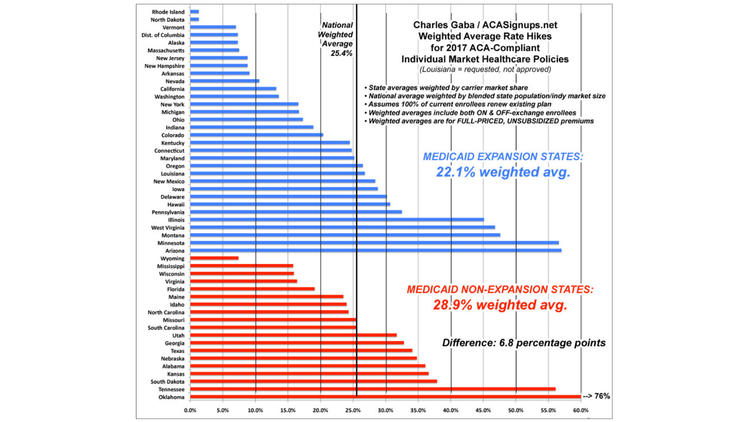
Charles Gaba, that indispensable tracker of ACA rates and policies, has fleshed out this phenomenon by comparing the weighted average premium increases for states that implemented the ACA cooperatively, even enthusiastically, with the increases in states that have resisted. (Gaba weights the increases by the enrollments of the insurance companies; in other words, a rate increase by a company with 100,000 customers counts more than one by a company with a few hundred customers.)
He finds that the weighted average rate increase for states that expanded Medicaid is 22.1% for 2017; among the 19 states that still have not expanded the program, it’s 28.9%. In states that formed their own marketplace to enroll Obamacare consumers, the increase is 17.3%; among those that rely on the federal government’s exchange, healthcare.gov, it’s 28%.
Finally, among states that refused to allow consumers to remain in pre-ACA insurance plans that didn’t comply with the new law as of 2014, the weighted average increase is 18.8%; among those that capitulated to hysteria over canceled pre-ACA insurance plans by grandfathering the non-compliant plans for as long as three years, it’s 28.4%.
Put these three factors together, and the states that fully embraced Obamacare will see increases of 18.2%. Those that fully resist will see increases of 29.8%.
The other complaint has been that many states are having their exchanges “implode” and people don’t have coverage because they don't have any insurers within their exchange, however as we move into the new year’s open enrollment period every state’s exchange does have at least one provider. But guess which of those states tended to have the fewest available providers?
 Available numbers of insurers on the Exchanges
Available numbers of insurers on the Exchanges
Here is is broken down county by county.
 County by County breakdown of Insurer participation in exchanges
County by County breakdown of Insurer participation in exchanges
So premiums have gone up — although not as much as they used to go up every year, in fact in some states and counties they have actually gone down — and insurers have left the market place, but in both cases those problems are generally worse in states that have resisted the ACA rather than those that have fully adopted it.
So we’re told we should “trust the laboratory of the states” that bills like Graham-Cassidy gives more power to the states to have flexibility and choices including dropping coverage for essential benefits, pre-existing conditions and allowing insurance companies to crank up their rates for those who want that kind of coverage — exactly why should we trust them since the consistent track record of many states have shown they have done far from their best to protect their citizens either from losing coverage or rapidly creeping prices, when they already had exactly the power to do both?
Just look what they’ve done with that power so far.
Now like anything else in the world it’s not an automatic rule that anything done by the States will always be either better or worse than what is done by the Federal Government. The only real difference is consistency, when you allow different choices within the states — you will naturally result in different results within those states, some will be worse but some will be better. Maybe we should be paying much more attention to the states that have better coverage, lower rates and stable markets, rather than giving the ones who don’t even more power to do more damage to repeat and worsen the mistakes they’ve already made.


